
Article reviewed by: Dr. Sturz Ciprian, Dr. Tîlvescu Cătălin and Dr. Alina Vasile
Article updated on: 04-04-2026
Everything you need to know about peptides: from the science of regeneration to research protocols
- What are peptides?
- Why peptides are of interest in cardiovascular medicine
- Injectable peptides: the most researched and most discussed
- Oral peptides: a biological challenge and a real promise
- Topical peptides: the most accessible and with the strongest human evidence
- Matrixyl (Palmitoyl Pentapeptide-4), the benchmark anti-aging peptide
- Argireline (Acetyl Hexapeptide-3) — the cosmetic alternative to botox
- Oral hydrolyzed collagen peptides — what internal supplementation brings
- GHK-Cu — the copper peptide with three decades of studies
- Topical Thymosin Beta-4 — the peptide that handles difficult wound healing
- Research peptides: promising in the lab, not yet certified for human use
- How hyperbaric therapy stimulates natural peptide production in the body
- Why hyperbaric therapy is the safe choice today
- The future of peptides: where research is heading
If you’ve recently heard about peptides at a clinic, online, or in a longevity podcast, and wondered what they are, whether they actually work, and if they are safe, you’re in the right place. Peptides have become one of the most discussed topics in modern medicine, and for good reason. Researchers are discovering that these tiny molecules, which our bodies naturally produce, have remarkable regenerative potential, from tissue healing and heart health to recovery after a stroke.
But before any enthusiasm, it is important to understand exactly what we know, what we don’t yet know, and where the boundary lies between promise and clinical reality. This article explains everything: the types of peptides, what medical studies say, how they are used, and, toward the end, why medical hyperbaric therapy remains, for now, one of the safest and best-documented options for heart and brain health.
What are peptides?
Think of the proteins in your body as long chains of links. Each link is an amino acid. A peptide is essentially a short fragment of such a chain, meaning a few links connected together, usually between 2 and 50 amino acids. When the chain becomes longer than 50, we are already talking about a protein.
What makes peptides special is not their small size, but the precision with which they act. Each peptide fits like a key into a specific lock, a receptor on the surface of cells, and sends a precise message: “build collagen”, “form new blood vessels”, “reduce inflammation”, “repair damaged tissue”. The human body naturally produces hundreds of such messengers. Insulin is a peptide. Oxytocin is a peptide. Growth hormone acts through peptides. The idea behind peptide therapy is simple: if these molecules already exist in the body and do beneficial things, can we use them or stimulate them therapeutically?
The answer from research is: yes, but with a lot of nuance.
Why peptides are of interest in cardiovascular medicine
The cardiovascular system is probably the field where peptides have shown the greatest regenerative potential. The reason is simple: the heart is an organ with an extremely limited capacity for self-regeneration. While the kidneys or liver can compensate to some extent, the heart cannot effectively replace the muscle cells lost after a heart attack. This is precisely where peptides come into play, as potential “architects” of a regenerative process that the body alone cannot complete.
And the epidemiological context makes this discussion urgent. According to National Institute of Public Health, cardiovascular diseases are responsible for nearly 56% of all recorded deaths in Romania. According to data from the Ministry of Health, the cardiovascular mortality rate in Romania is 2.5 times higher than the European Union average.
And hypertension, one of the main risk factors, affects over 45% of adults in Romania, according to the Romanian Society of Hypertension. These numbers are not abstract statistics. They describe a public health crisis in which any new therapeutic option deserves to be taken seriously.
Injectable peptides: the most researched and most discussed
Injectable peptides are the category with the largest volume of research and, at the same time, the greatest interest from informed audiences. The reason injection is preferred over swallowing a pill is simple: our stomach breaks down peptides like any other protein. Digestive enzymes break them into pieces before the active molecule reaches the bloodstream. Subcutaneous (under the skin) or intramuscular injectable administration bypasses this problem and allows the peptide to reach circulation intact.
BPC-157 — the peptide from gastric juice
If you had to choose a single peptide that has generated the greatest wave of interest in medical research over the past decade, it would almost certainly be BPC-157. Not because it has the most spectacular name, the abbreviation comes from “Body Protective Compound 157”, but because the spectrum of effects documented in studies is unusually broad for such a small molecule.
Its origin is, at first glance, surprising: it is a sequence of 15 amino acids derived from a protein naturally present in human gastric juice. Our stomach produces it constantly, and over time researchers have observed that the digestive tract has a remarkable ability to heal quickly after injury. The natural question was: could BPC-157 be related to this ability? And if so, can it be used in other tissues?
The answer from research so far is, with appropriate caution, yes. A systematic analysis published in 2025 by researchers at Case Western Reserve University, in HSS Journal, "Emerging Use of BPC-157 in Orthopaedic Sports Medicine", reviewed 544 articles and included 36 studies. The conclusion? BPC-157 stimulates VEGF production (vascular endothelial growth factor), activates cellular proliferation pathways, and reduces inflammatory cytokines, the molecules that sustain chronic inflammation. Simply put: this peptide seems to tell cells: build new blood vessels, multiply, and stop the inflammatory fire. All three are crucial processes after a heart attack or any other tissue injury.
Another study published in 2025 in PMC, "Regeneration or Risk? A Narrative Review of BPC-157", confirms that BPC-157 stimulates nitric oxide production, a molecule that blood vessels naturally use to dilate and allow better flow. When vessels produce too little nitric oxide (as happens in atherosclerosis, diabetes, or hypertension), blood flows more poorly, blood pressure rises, and heart attack risk increases. BPC-157 appears capable of reactivating this natural pathway.
A 2025 study, "Protective Effects of BPC-157 on Liver, Kidney, and Lung Following Lower Extremity Ischemia-Reperfusion", showed that the peptide protected the liver, kidneys, and lungs from damage caused by lack of blood and its sudden return, a mechanism known as “reperfusion injury”, which we will discuss later in the context of heart attack.
All of this sounds promising. And it is. But there is an essential nuance that any honest article must clearly state: BPC-157 is not approved as a medication in the European Union or by the FDA for any human indication. All the studies mentioned are conducted on animals. BPC-157 is legally marketed exclusively as a research substance, meaning for laboratory use, not for human consumption. Its long-term safety profile in humans is unknown. However, this does not diminish the value of the research, but it means that any decision to use it cannot be made without careful medical supervision and a clear understanding of the current evidence limitations.
TB-500 and Thymosin Beta-4, the alarm signal of blood vessels
There is a remarkable biological emergency system in the body: when a tissue is injured, the cells around the wound emit chemical signals that “call” repair cells from other parts of the body, including the bone marrow, where stem cells are stored. Thymosin Beta-4 is one of the molecules that coordinates this mobilization. It is naturally produced by the thymus, an immune gland located behind the sternum, roughly the size of a fig, and plays a central role in mobilizing endothelial progenitor cells, those “pre-vascular” cells capable of contributing to the repair of damaged blood vessels. TB-500 is a synthetic version of its active fragment, designed to replicate this mobilization and repair function.
A study published in 2024 in the journal Angiogenesis, "Restoration of Blood Vessel Regeneration in the Era of Advanced Therapies", documents that Thymosin Beta-4 stimulates the migration of endothelial cells to damaged areas, reduces vascular wall inflammation, and promotes the formation of new capillaries. Capillaries are the smallest blood vessels in the body, an invisible network to the naked eye, but essential because they supply individual cells. When a heart attack or a stroke destroys this fine network, tissues no longer receive oxygen and glucose, even if the large arteries are reperfused. Thymosin Beta-4 could help rebuild this fine network, an effect that no current therapy directly addresses.
A study published in PLOS ONE demonstrated that TB-4 applied in experimental models increased wound re-epithelialization by up to 61% compared to the control group, with a significant increase in collagen deposition and local angiogenesis. The stimulation of migrating cells that cover and protect the skin was 2 to 3 times higher than in the untreated group, at extremely low doses in the picogram range. This suggests that TB-4 acts as a low-amplitude signal with a disproportionately large biological effect relative to the administered amount.
Like BPC-157, TB-500 is marketed exclusively for research and has no authorization for therapeutic use in humans in the EU or USA
CJC-1295 and Ipamorelin, peptides that stimulate growth hormone
So far we have discussed peptides that act directly on tissues, meaning blood vessels, muscles, skin. However, there is another category of peptides with a completely different mechanism: instead of repairing directly, they activate the pituitary gland. This is a small gland at the base of the brain, about the size of a pea, which coordinates the production of several essential hormones, including growth hormone (GH). CJC-1295 and Ipamorelin are two peptides that stimulate the pituitary to produce more GH, each through slightly different but complementary mechanisms.
CJC-1295 mimics a natural brain signal that tells the pituitary to produce more growth hormone, prolonging and amplifying this signal beyond what the body can produce on its own. Ipamorelin does the same but with greater selectivity. It stimulates GH release without disrupting other pituitary hormones such as cortisol or prolactin. Their combination is frequently studied precisely because their effects can enhance each other.
Why does growth hormone matter for the heart? Because GH supports muscle mass, including the myocardium, which is also a muscle, promotes fat metabolism, and has direct effects on cardiac function. In patients with heart failure or GH deficiency, low levels of this hormone are associated with a worse prognosis. A 2025 analysis published on DrOracle confirms that Ipamorelin is safer than other GH secretagogues precisely because it does not interfere with cortisol or prolactin, hormones whose increase can generate significant adverse effects.
From a regulatory standpoint, the situation is similar to the other peptides discussed: CJC-1295 and Ipamorelin do not have approved indications for general human use in the EU and are marketed exclusively as research substances. There are specific clinical contexts in which GH secretion is studied, but the standardization of human therapeutic protocols is, for now, incomplete.
Endogenous cardiac peptides - produced by the heart to protect itself
Not all peptides relevant to the heart are synthetic substances from research laboratories. Some are produced by the heart itself, as its own alarm and protection system. B-type natriuretic peptides (BNP, meaning brain natriuretic peptide, despite the name, produced by the heart) are released by the myocardium when it is under strain. One example of this is heart failure. Their elevated level in the blood functions as a biological alarm signal and is now used in clinical practice as a diagnostic marker. But the role of BNP is not passive: it actively inhibits myocardial fibrosis (that is, the transformation of heart tissue into rigid scar tissue) and modulates inflammation. That is precisely why the drug Entresto, approved for heart failure, works in part by amplifying the effects of endogenous natriuretic peptides.
A review published in 2024 in Frontiers in Pharmacology, "Peptides Are Cardioprotective Drugs of the Future", analyzes a broad spectrum of peptides with cardioprotective potential and concludes that cardiovascular medicine is clearly moving toward therapies that mimic or enhance the body’s natural mechanisms of cardiac protection, including through synthetic peptides designed to imitate active biological sequences.
Oral peptides: a biological challenge and a real promise
Patients often ask for treatment that is simple to manage, which in most cases means a pill. Unfortunately, when it comes to peptide treatment, this simplicity is more nuanced. The fundamental problem is that the stomach treats a peptide just like any other protein in food, meaning it breaks it down into its individual amino acids. A BPC-157 pill, for example, reaches the stomach, is dissolved by digestive enzymes, and enters the bloodstream not as an active peptide, but as simple amino acids, which obviously no longer have the same effect.
However, there are oral peptides with documented cardiovascular effects, especially from food sources. A European Union-funded research program, the BACCCHUS Project (CORDIS), demonstrated that bioactive peptides from foods such as fish, egg white, wheat, or dry-cured ham can help lower blood pressure, improve lipid profiles, and increase nitric oxide production (the natural vasodilator mentioned above), with measurable beneficial effects in randomized controlled human studies.
Modern pharmacology is also advancing toward special formulations that protect synthetic peptides from digestive degradation, such as nanoparticles, liposomes, or enzyme inhibitors administered simultaneously. Oral semaglutide (the tablet version of Ozempic), already approved in the EU for diabetes and weight management, demonstrates that this barrier can be overcome, even if the road remains long for other molecules.

Topical peptides: the most accessible and with the strongest human evidence
Direct application to the skin is the simplest route of peptide administration, and, surprisingly, the field with the most already validated clinical applications. Cosmetic peptides have moved in less than two decades from the niche of biochemistry laboratories into the daily skincare routine of millions of people.
Why does the topical route work for peptides, when we have seen that the oral route has major limitations? Small-molecule peptides can penetrate the stratum corneum, meaning the superficial layer of the skin, and reach the dermis, the deeper layer where fibroblasts are found. Fibroblasts are the skin’s factory cells: they produce collagen, elastin, and hyaluronic acid, precisely the molecules responsible for firmness, elasticity, and hydration. There, peptides for skin deliver precise biological messages: “produce more collagen,” “form new vessels,” “repair the skin barrier,” “calm inflammation.” Aging or damaged skin does not receive these instructions in sufficient quantity, and topical peptides reintroduce them from the outside.
Matrixyl (Palmitoyl Pentapeptide-4), the reference anti-aging peptide
Matrixyl is probably the most studied anti-aging cosmetic peptide in the world. Its trade name is used for palmitoyl pentapeptide-4, a synthetic molecule designed to mimic fragments of degraded collagen. In this way, it tricks the skin into sensing broken collagen, in order to stimulate it to produce new collagen in compensation.
Clinical studies on Matrixyl are consistent: a formulation based on palmitoyl pentapeptide-4 demonstrated a reduction in wrinkle depth of up to 45% compared to the placebo group, after 8–12 weeks of daily use, according to data summarized by Peptide Journal. L'Oréal Paris, one of the largest cosmetic manufacturers in the world, cites a study showing that peptides can stimulate collagen production in the skin by up to 30% when applied topically, with visible effects in reducing wrinkles and improving firmness. Matrixyl 3000, an improved variant combining palmitoyl tetrapeptide-7 with palmitoyl oligopeptide, has demonstrated comparable or superior results, with additional benefits in reducing low-grade chronic inflammation associated with skin aging.
From a mechanistic perspective: Matrixyl does not act directly on wrinkles, but rebuilds the structure of which wrinkles are the symptom. This is a profoundly different type of approach compared with classic moisturizers, which temporarily plump the skin, or with filler procedures, which add volume from the outside. Matrixyl persuades the skin to rebuild its own support structures.
Argireline (Acetyl Hexapeptide-3) — the cosmetic alternative to botox
Argireline is often called “botox in a cream,” a comparison that simplifies things, but is not entirely wrong. The mechanism is similar: botox blocks the release of acetylcholine (the chemical substance through which nerves command muscles to contract), temporarily paralyzing the facial muscles that produce expression lines. Argireline acts through a similar but gentler mechanism, interfering with the SNARE complex, meaning the molecular mechanism through which neurons release neurotransmitters, partially reducing the intensity of facial muscle contractions, without the paralytic effect of botulinum toxin.
A randomized, placebo-controlled study published in the International Journal of Cosmetic Science, "A synthetic hexapeptide (Argireline) with antiwrinkle activity", demonstrated that Argireline is a non-toxic peptide with anti-wrinkle activity mechanically comparable to botulinum toxin, but without neurotoxicity. A second clinical study published in Skin Research and Technology, "The anti-wrinkle efficacy of argireline", evaluated 60 subjects who applied Argireline to periocular wrinkles (those around the eyes) twice a day for four weeks. Result: 48.9% of the treated group showed anti-wrinkle improvement versus 0% in the placebo group, with significant reduction in objectively measured roughness parameters.
The advantage over botulinum toxin is obvious: Argireline is applied at home, without injections, without the risk of asymmetric paralysis, and without the cost of repeated medical procedures. The disadvantage, equally real: the effects are more moderate and disappear once use is discontinued, Argireline does not rebuild the skin’s structure, but temporarily reduces the muscle contractions that deepen expression lines. The best candidates for this peptide are people with expression wrinkles (forehead, corners of the eyes, perioral area), not wrinkles caused by collagen loss or prolonged sun exposure.
Oral hydrolyzed collagen peptides — what internal supplementation brings
Beyond direct topical application, orally administered collagen peptides have gained enormous popularity in recent years and, exceptionally compared to other oral peptides, there are human clinical studies that partially support this popularity. Hydrolyzed collagen (meaning collagen broken down into small, absorbable peptides) has demonstrated measurable skin benefits in multiple randomized controlled studies.
A clinical study conducted on 105 women between the ages of 24 and 50 who consumed collagen peptides for six months documented smoother, more elastic skin with visibly improved appearance in all participants. Studies with hydrolyzed PEPTAN collagen showed that after 12 weeks of supplementation, collagen density in the dermis increased by 8.83% compared to the placebo group, where no change was recorded. Why does oral collagen work, even though we said peptides degrade in the stomach? Precisely because hydrolyzed collagen peptides are already pre-digested into small fragments, dipeptides and tripeptides that can be absorbed relatively intact through the intestinal mucosa and enter circulation, where they stimulate fibroblasts in the dermis to produce their own collagen.
GHK-Cu — the copper peptide with three decades of studies
GHK-Cu (glycyl-L-histidyl-L-lysine-copper) is one of the most studied topical peptides in the history of biochemistry. It is a tripeptide, meaning a peptide made of only three amino acids, naturally present in the blood plasma of young people. At age 20, its blood level is around 200 ng/mL; at age 60, it drops to 80 ng/mL. Researchers observed that this decline coincides with the loss of tissue regenerative capacity with age.
A study published in the International Journal of Molecular Sciences in 2018, "Regenerative and Protective Actions of the GHK-Cu Peptide", documented that GHK-Cu stimulates the growth of blood vessels and nerves, increases collagen and elastin production, reduces inflammation, and activates the tissue antioxidant system. Moreover, a controlled clinical study with 71 women showed that a facial cream with GHK-Cu applied for 12 weeks increased dermal density and thickness, reduced wrinkles, and improved skin texture, with results superior to vitamin C or retinoic acid in collagen production.
Topical Thymosin Beta-4 — the peptide that handles difficult wound healing
Thymosin Beta-4, applied topically directly to a wound or skin lesion, has demonstrated remarkable effects in research models. A study published in 2024 in the Journal of Tissue Engineering, "Discovery of Bioactive Peptides as Therapeutic Agents for Skin Wound Repair", documents that TB-4 increased re-epithelialization (meaning the covering of the wound with new skin) and local angiogenesis, with notable activity in stimulating the migration of repair cells toward the injured area. This is a valuable property for chronic wounds such as diabetic ulcers, pressure sores, or post-radiation wounds, which represent a major clinical problem where current therapeutic options are limited.
Research peptides: promising in the lab, not yet certified for human use
It is time to clarify an aspect that the internet often treats ambiguously: the legal and medical status of many of the peptides discussed above.
In the European Union, a substance can be administered to humans as a medicine only if it has received authorization from the EMA (European Medicines Agency), after completing Phase I, II, and III clinical trials that demonstrate both safety and efficacy. Peptides such as BPC-157, TB-500, CJC-1295, or Ipamorelin do not have this authorization. They may be legally produced and sold as “research substances,” which means they are intended exclusively for laboratory use, not human consumption.
An article published in 2026 regarding the evolution of the European peptide market shows that European authorities have intensified oversight of companies that label these substances as “research only,” but clearly promote them for human consumption. This is a real problem: the lack of regulation means that purity, exact concentration, and absence of contaminants are not guaranteed by any certification body.
The correct attitude toward these molecules is neither total rejection nor uncritical enthusiasm. Their research is promising and deserves to continue. But at present, their human administration outside a controlled research protocol involves unknown risks. A responsible physician cannot recommend their use in standard clinical practice, precisely because of the absence of complete clinical evidence in humans.
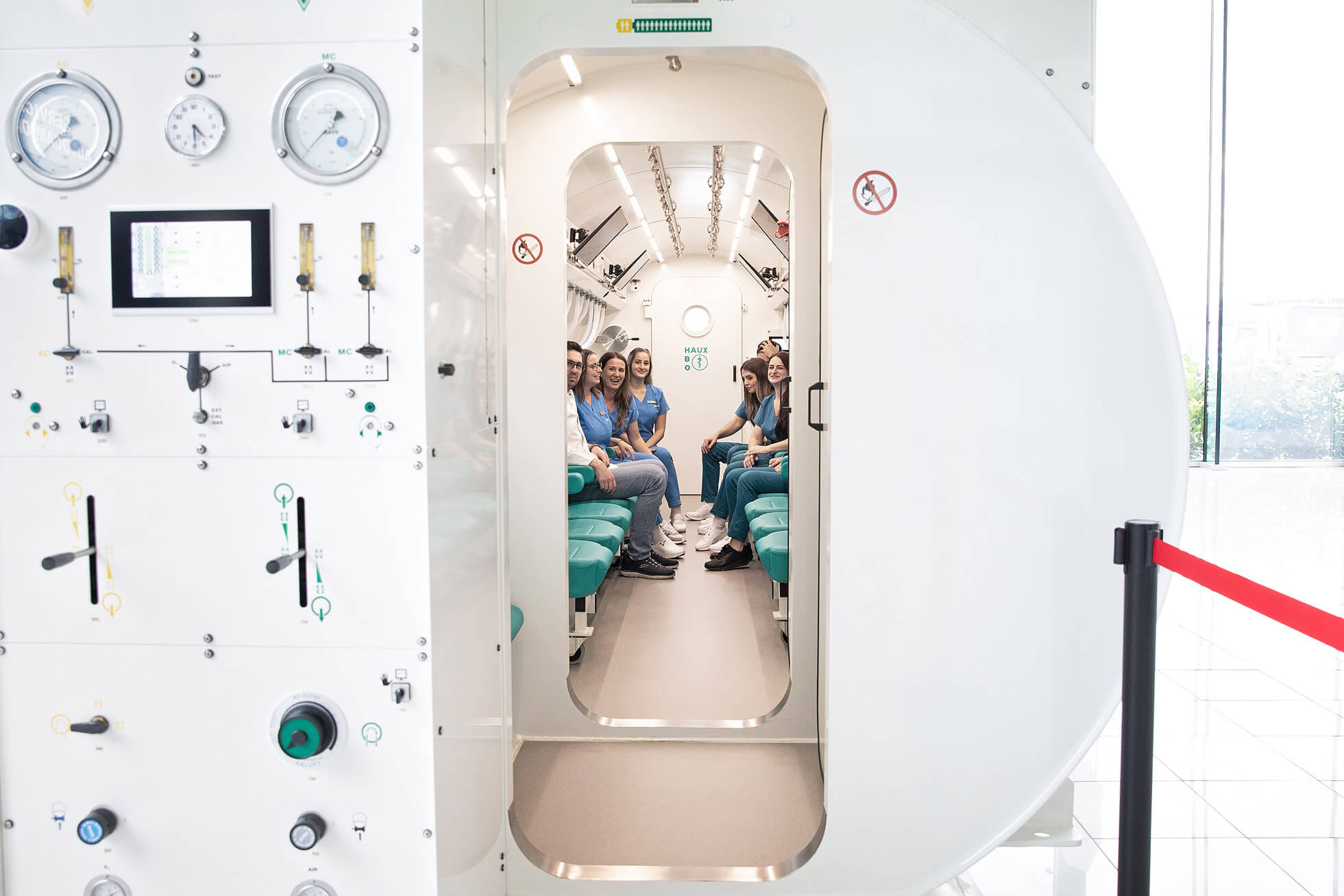
How hyperbaric therapy stimulates natural peptide production in the body
There is a way to access the biological mechanisms of regenerative peptides without the risks of an unauthorized product: by stimulating their production by the body itself. Medical hyperbaric therapy does exactly this, with decades of human clinical evidence behind it.
When a patient enters a hyperbaric chamber and breathes 100% oxygen at a pressure 2–3 times higher than normal, the body does not receive a chemical substance from the outside. It receives a precise physical signal, to which it responds by producing the molecules it needs for repair. VEGF, the factor that commands the formation of new blood vessels in ischemic areas. BDNF, the factor that nourishes and protects neurons after a stroke or neurological injury. SDF-1, the molecule that functions as a navigation system for stem cells, calling them from the bone marrow exactly to the injured area. All of these are endogenous peptides and growth factors, meaning produced by the body, not introduced from outside.
What is remarkable from the perspective of peptide research is that these are exactly the molecules scientists are trying to reproduce synthetically in laboratories. BPC-157 stimulates VEGF. TB-500 mobilizes progenitor cells toward injured areas, similar to SDF-1. CJC-1295 activates a hormonal cascade that supports tissue repair. Hyperbaric therapy activates all of these processes simultaneously, not by introducing external molecules of uncertain status, but by creating the conditions in which the body produces them itself, in doses it regulates naturally and under continuous medical supervision. It is not a compromise alternative to synthetic peptides. In many respects, it is the original mechanism that peptide science is trying to imitate.
Why hyperbaric therapy is the safe choice today
The peptides we have discussed in this article, BPC-157, TB-500, CJC-1295, Ipamorelin, have one thing in common: laboratory results are promising, but studies in humans are still insufficient for any physician to recommend them as treatment. This does not mean the science behind them is wrong. It simply means that the path from animal testing to safely treating humans is long, costly, and, for many of these molecules, still not fully completed. Until that path is completed, they remain substances intended for research, not human consumption.
Hyperbaric therapy is in a completely different position. It is not a novelty and it is not a promise, it is a medical method used for more than six decades in hospitals and clinics around the world, with hundreds of studies carried out on real human patients and with protocols officially recognized by European and international medical bodies. A review article published in 2025 in PMC, "Application and Progress of Hyperbaric Oxygen Therapy in Cardiovascular Diseases", documents that hyperbaric therapy protects the heart muscle after a heart attack, stimulates the formation of new blood vessels in affected areas, and improves the ability of vessels to function normally. All of these are effects measured in humans, not only in animal experiments.
In stroke recovery, the results are just as clear. A study published in PLOS ONE in 2013, "Hyperbaric Oxygen Induces Late Neuroplasticity in Post Stroke Patients", showed something remarkable: patients with neurological deficits remaining after a stroke, two years after the event, meaning during a period when the brain no longer recovers spontaneously, showed real improvements after 40 sessions of hyperbaric therapy. Moreover, brain imaging showed that areas of the brain that were no longer functioning had “reactivated.” This is called neuroplasticity, the brain’s ability to form new connections, and it is essentially the basis of any neurological recovery.
Another concrete advantage of hyperbaric therapy is that you know exactly what you are receiving. According to StatPearls / NIH, “Hyperbaric Cardiovascular Effects,” the effects of hyperbaric therapy are well documented and reproducible: oxygen dissolves in the blood in amounts up to 20 times greater than normal, reaching tissues even where circulation is poor, with well-characterized anti-inflammatory and regeneration-stimulating effects. In a certified medical clinic such as Hyperbarium, each session takes place with 100% oxygen, at a standardized pressure, with verified equipment and under continuous medical supervision. There are no surprises regarding product quality or dose, real issues in the case of research peptides bought online, where no one guarantees that the vial contains exactly what the label says.
The future of peptides: where research is heading
Research on therapeutic peptides is, in 2025–2026, at an interesting moment. We are no longer in the phase where scientists are just discovering that these molecules exist and that they can do remarkable things.
Several molecules are already in Phase I and II clinical trials, meaning they are being tested in humans for the first time, in small groups of volunteers, to assess safety and optimal doses. Others are in the formulation optimization phase: researchers are looking for solutions to make them stable, absorbable, and conveniently administrable, without losing their biological activity. A study published in Biomolecules in 2025, "Bioactive peptides: from preclinical to clinical studies", identifies several priority directions: peptides that help control cholesterol, peptides with direct anti-inflammatory effects on blood vessels, and peptides that modulate hormonal systems with broad metabolic impact. All these are areas in which highly prevalent chronic diseases such as cardiovascular disease, diabetes, and obesity urgently need new solutions.
In the field of skincare, progress is already visible. New variants of GHK-Cu and extracellular matrix peptides are being evaluated for advanced medical formulations, beyond cosmetics, in the treatment of chronic wounds, pathological scars, and inflammatory dermatological conditions. In oncology, antimicrobial peptides and immune-signaling peptides represent an active frontier, with several molecules already in clinical trials for certain types of cancer. In neurology, neurotrophic peptides, molecules that nourish and protect neurons, are being studied as potential tools in Alzheimer’s, Parkinson’s, and post-traumatic recovery.
There is also a structural obstacle that peptide research must overcome: many of the most promising compounds cannot be patented, because they are derived from natural biological sequences. Without a patent, pharmaceutical companies have reduced financial incentives to invest hundreds of millions of euros in full clinical trials. This is, paradoxically, one of the reasons why some peptides with excellent preclinical results remain in the research zone for years, not because the science is weak, but because the economic model of clinical research does not favor molecules that cannot become the exclusive property of one company.
What is certain is that peptides are not a passing trend. They are part of the fundamental biology of every living organism, and understanding how they can be used therapeutically will continue to advance. Some will become approved medicines. Others will remain in the world of cosmetics and supplements with solid evidence. And others, the most complex ones, will wait a few more years until human clinical trials confirm or disprove the promises seen in the lab. Until then, the best thing an informed patient can do is understand the distinction between evidence and promises, and make any therapeutic decision together with a physician who understands both the potential and the limitations of this fascinating field.




