
Article reviewed by: Dr. Sturz Ciprian, Dr. Tîlvescu Cătălin and Dr. Alina Vasile
Article updated on: 13-03-2026
How hyperbaric therapy can support recovery after heart diseases
- What hyperbaric therapy means for the heart
- What happens in the body during a hyperbaric therapy session
- How hyperbaric oxygen therapy can help after a myocardial infarction
- Heart failure: when the heart becomes exhausted over time
- Peripheral arterial disease and diabetic angiopathy
- Refractory angina pectoris: pain that does not respond to standard treatment
- Stroke and neurological recovery
- Possible side effects: what is important to know
- How to maintain cardiovascular health
- Why an individualized approach matters
- What hyperbaric therapy can and cannot do for the heart
- Hyperbaric oxygen therapy for a healthy heart – additional support on the road to recovery
Cardiovascular diseases remain the greatest medical challenge of modern times, being responsible for approximately one third of all global deaths. According to the World Health Organization, around 19.8 million people died from cardiovascular diseases in 2022, of which 85% were caused by myocardial infarction and stroke. In Romania, the situation is even more alarming: in 2023, the standardized mortality rate from cardiovascular diseases was 2.5 times higher than the European Union average, with 600.8 deaths per 100,000 inhabitants. Approximately 1 in 2 people in Romania died due to diseases of the circulatory system, with 43,460 deaths from ischemic heart disease and 42,826 deaths caused by cerebrovascular diseases reported in 2023.
In this dramatic context, modern medicine constantly explores new ways to support the recovery process after acute cardiovascular events. One of the adjunct therapies that has attracted the attention of the international medical community in recent years is hyperbaric oxygen therapy (HBOT - Hyperbaric Oxygen Therapy). Although it is not a standalone cardiological treatment, this therapy can play an important role in recovery after certain heart diseases, being integrated into a complex and personalized therapeutic plan.
What hyperbaric therapy means for the heart
Hyperbaric therapy for the heart involves administering pure oxygen at a pressure higher than the normal air we breathe. The treatment takes place in a special chamber called a hyperbaric chamber, where pressure is increased in a controlled way, similar to what we feel when an airplane ascends or descends, but under safe and medically supervised conditions.
Normally, oxygen is transported in the blood bound to hemoglobin in red blood cells. When we breathe oxygen under increased pressure, a much larger amount of oxygen dissolves directly into the plasma, the liquid component of the blood. This has several important consequences: more oxygen reaches hard-to-access areas, including tissues with compromised vascularization; atrophied or senescent cells, which are not dead but do not function properly due to lack of oxygen, can receive real support; at the same time, small blood vessels receive signals to repair themselves and, in some cases, to form new structures.
In short, hyperbaric therapy for the cardiovascular system helps the body deliver oxygen to areas where circulation has been affected. For the heart and blood vessels, this therapy can make a difference in the recovery process.
At Hyperbarium, the hyperbaric chamber is a modern multiplace medical device with a capacity of up to 16 people. It is manufactured in Germany and classified as a Class IIB medical device, meaning it meets strict European safety and quality standards. The working pressure can reach up to 3 ATA (absolute atmospheres), and the chamber is equipped with advanced ventilation and cooling systems for thermal comfort, viewing windows, communication systems with the medical team, and appropriate lighting. An important advantage of the multiplace configuration is that medical staff can enter the chamber together with patients, which means direct supervision throughout the treatment and significantly greater safety.
What happens in the body during a hyperbaric therapy session
To understand why hyperbaric therapy can help the heart and blood vessels, it is useful to see how it works at the biological level, explained as simply as possible.
Cells of the heart and blood vessels need oxygen to produce energy and function normally. When oxygen supply is reduced, due to a blocked, narrowed, or diseased vessel, cells begin to suffer. Some die. Others survive but have reduced activity: they consume less, produce less, and do not function as they should. Doctors call this condition “myocardial hibernation” or “myocardial stunning,” and it explains why heart function may remain below optimal levels even after a heart attack has been properly treated.
When oxygen is administered under increased pressure, 10–15 times more oxygen dissolves in the blood than under normal conditions. This oxygen also reaches areas with impaired microcirculation, where red blood cells cannot easily penetrate. Once there, oxygen can reactivate hibernating cells, support endothelial repair (the inner lining of blood vessels), reduce local inflammation, and stimulate healing processes.
Another mechanism is the stimulation of new blood vessel formation (angiogenesis). Hyperbaric therapy triggers the release of growth factors, including VEGF (vascular endothelial growth factor), which stimulates the formation of new capillaries and arterioles in ischemic areas. In other words, the body is encouraged to build alternative blood routes where existing vessels are compromised. This mechanism is particularly useful in peripheral vascular diseases and post-infarction recovery.

How hyperbaric oxygen therapy can help after a myocardial infarction
Myocardial infarction, commonly known as a “heart attack,” occurs when a coronary artery suddenly becomes blocked and part of the heart muscle is deprived of blood and oxygen. Emergency treatment, meaning reopening the artery through stenting or thrombolysis, is absolutely essential. Without it, hyperbaric therapy has no role and cannot compensate for the lack of cardiological intervention.
Data from Romania shows that 43,460 people died from ischemic heart disease in 2023, and the standardized cardiovascular mortality rate is 2.5 times higher than the European Union average. This means that in Romania, heart attacks often strike earlier, more severely, and with fewer recovery resources.
After the artery has been reopened, the story does not end. In the affected area, some cardiac cells die and will never regain their function. Others, however, remain in distress: they survive but do not work at full capacity because they have gone through a severe episode of oxygen deprivation. This is exactly where hyperbaric oxygen therapy can come into play.
A study published in “Cardiovascular Drugs and Therapy” evaluated patients with acute infarction who received, in addition to standard thrombolysis treatment, sessions of hyperbaric therapy. The results showed that in the group treated with hyperbaric oxygen, enzymes that reflect cardiac cell damage increased less and normalized faster. In addition, the pumping function of the heart, expressed by the ejection fraction, was better at discharge in the group that received hyperbaric therapy (52.4% compared to 47.3% in the group without this therapy). Simply put, the heart muscle suffered less damage.
Other research has confirmed this direction. In patients with myocardial infarction treated through primary percutaneous coronary intervention, the use of hyperbaric therapy was associated with improved tissue perfusion and an increase in ejection fraction after the procedure. Experimental studies have also shown that hyperbaric therapy improves the antioxidant balance of cardiac cells and reduces markers of oxidative stress, thus protecting tissues surrounding the infarcted area.
It is important to remember that hyperbaric therapy for heart diseases in the case of myocardial infarction always represents a complementary approach. It does not replace angiography, stents, antiplatelet medication, statins, or cardiac rehabilitation programs, but is added to them.
Heart failure: when the heart becomes exhausted over time
Heart failure is a chronic disease in which the heart can no longer pump enough blood to meet the body’s needs. Patients become easily fatigued, experience shortness of breath during effort or even at rest, have swelling in their legs or abdomen, and may wake up at night feeling like they are suffocating. It is a condition that significantly changes quality of life and requires carefully dosed and monitored medication.
In Romania, heart failure affects approximately 560,000 people, meaning nearly 5% of adults. The standardized mortality rate is twice as high as in other European Union countries, according to data from the Romanian Society of Cardiology. More than half of diagnosed patients die within the first 5 years. These figures show how important not only medication is, but also proper and complete recovery.
Basic treatment includes medication (ACE inhibitors or sartans, beta-blockers, diuretics, antialdosterones), lifestyle changes, and sometimes implantable devices or surgical interventions. Hyperbaric therapy may represent a valuable addition in certain cases.
Recent research has shown that in patients with coronary artery disease and impaired ventricular function, hyperbaric oxygen therapy sessions can improve the left ventricular ejection fraction, which is the main indicator of the heart’s pumping power. A meta-analysis published in 2025 in the “British Journal of Cardiology” demonstrated that hyperbaric therapy administered after coronary revascularization significantly increased this ejection fraction compared with patients who did not receive the therapy. This does not represent a complete “repair” of the heart, but rather concrete help in areas where heart muscle is still alive yet poorly perfused and functioning below capacity.
At Hyperbarium, patients with heart failure are evaluated by a cardiologist before starting any protocol. Severe heart failure requires caution: pressure changes can be demanding for a very weakened heart. That is why a prior medical consultation is mandatory to determine who can safely benefit and who first needs stabilization.
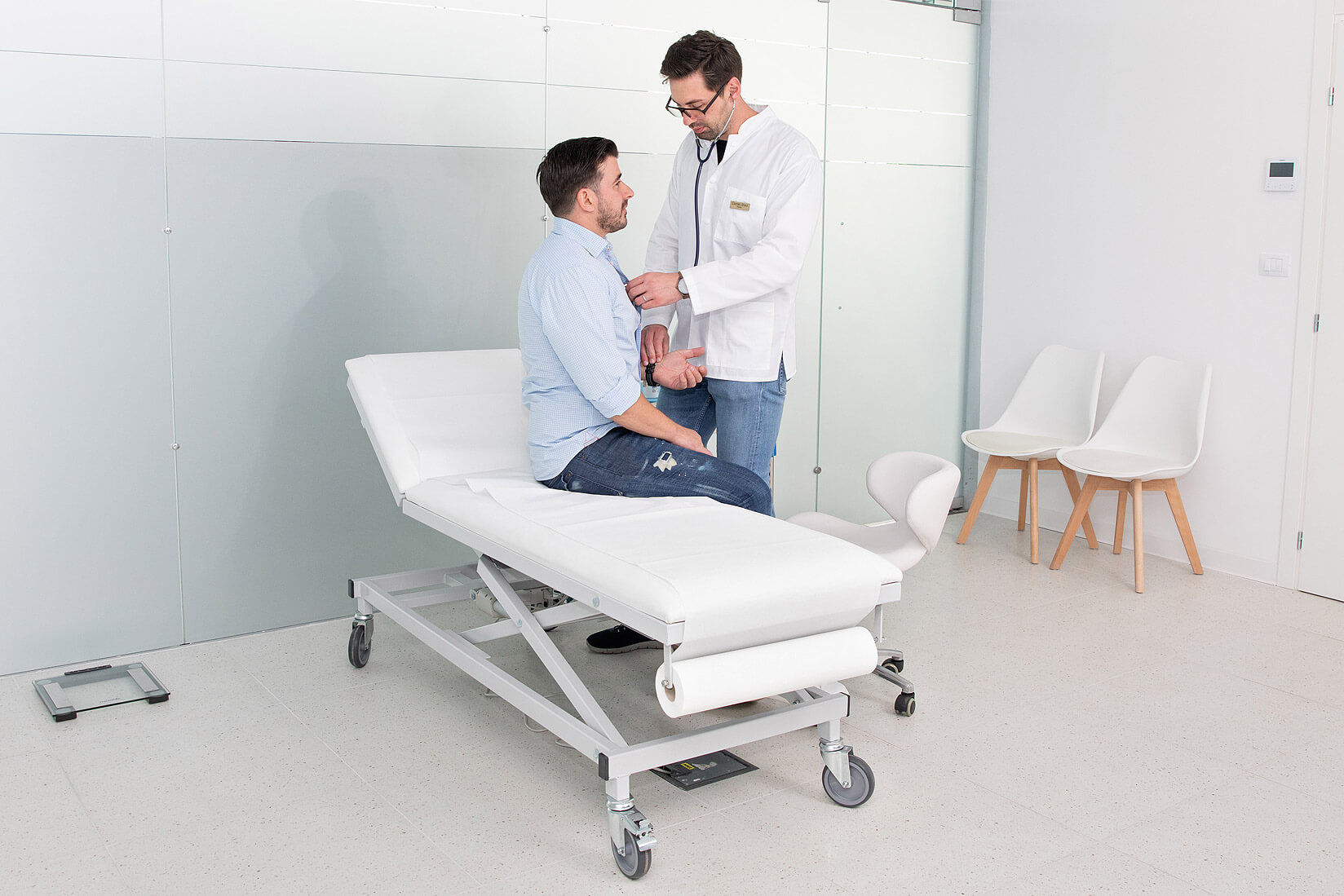
Peripheral arterial disease and diabetic angiopathy
Atherosclerosis does not affect only the arteries of the heart. Deposits of fat and calcium on arterial walls can occur throughout the entire vascular system, including in the arteries of the legs. Peripheral arterial disease is the form experienced in the limbs: pain while walking that forces a person to stop, a cold sensation in the feet, wounds that do not heal, and changes in skin color and temperature. In advanced stages, the risk of gangrene and amputation becomes real.
The situation becomes even more complex in patients with diabetes mellitus. Recent data shows that approximately 1 in 12 Romanians has diabetes, and many cases are still undiagnosed. Diabetes accelerates atherosclerotic processes and affects both large and small blood vessels, leading to what is known as diabetic angiopathy. The combination of damaged nerves, narrowed vessels, and impaired healing makes ischemic diabetic foot one of the most difficult complications to manage.
Heart diseases and peripheral circulation diseases are connected through the same basic mechanism: lack of oxygen in tissues. This is where hyperbaric therapy for heart diseases intervenes, through two main mechanisms. The first is the direct increase in oxygen availability in ischemic areas, even where circulation is compromised. The second is stimulation of new vessel formation by mobilizing endothelial progenitor cells—young cells capable of building endothelium (the inner lining of vessels) and contributing to the development of new capillaries.
A prospective study on patients with peripheral arterial disease showed that after series of hyperbaric therapy sessions at 3 ATA, the level of endothelial progenitor cells increased significantly in the blood. At the same time, angiogenic markers (growth factors that stimulate new vessel formation) also increased considerably. The most important clinical result was the improvement of skin perfusion pressure—an indicator of blood flow at the surface of the skin of the foot—and the fact that none of the participants required amputation during the study.
Another study evaluated the effect of hyperbaric therapy in patients with occlusive arterial disease and diabetic angiopathy and observed a reduction in fibrinogen (a marker of inflammation and thrombotic risk) and significant clinical improvement compared with the untreated group. Oxygen under increased pressure helps normalize vascular functions, create an environment that inhibits anaerobic bacteria, and stimulate fibroblasts and collagen synthesis processes—the essential ingredients for healing.
For patients with diabetic foot ulcers, hyperbaric therapy for the cardiovascular system is internationally recognized as a complementary treatment with strong scientific evidence for precisely these reasons.
Refractory angina pectoris: pain that does not respond to standard treatment
There is a category of cardiovascular patients who, although they have received optimal medication and undergone revascularization procedures, continue to experience frequent chest pain, known as angina pectoris. This condition is called refractory angina and is estimated to affect hundreds of thousands of people worldwide. The quality of life of these patients is severely affected: they cannot perform physical effort, fear every episode of chest pain, and often develop chronic anxiety.
In such cases, hyperbaric therapy is being studied as a supportive option. By improving coronary microcirculation—meaning the small blood vessels within the heart muscle—and by stimulating the formation of collateral vessels (alternative vascular pathways that bypass blocked areas), hyperbaric oxygen therapy may help reduce the frequency and intensity of painful episodes.
The mechanism is similar to that in peripheral arterial disease: where large vessels can no longer be revascularized, the body may be supported in building an alternative network of small vessels. It is not a perfect solution, but it can make the difference between being able to walk a few hundred meters without pain and being limited to only a few steps.
It is important to clarify that refractory angina requires full cardiological evaluation and that any decision regarding hyperbaric therapy in this context should be made together with a cardiologist, based on the individual clinical picture.
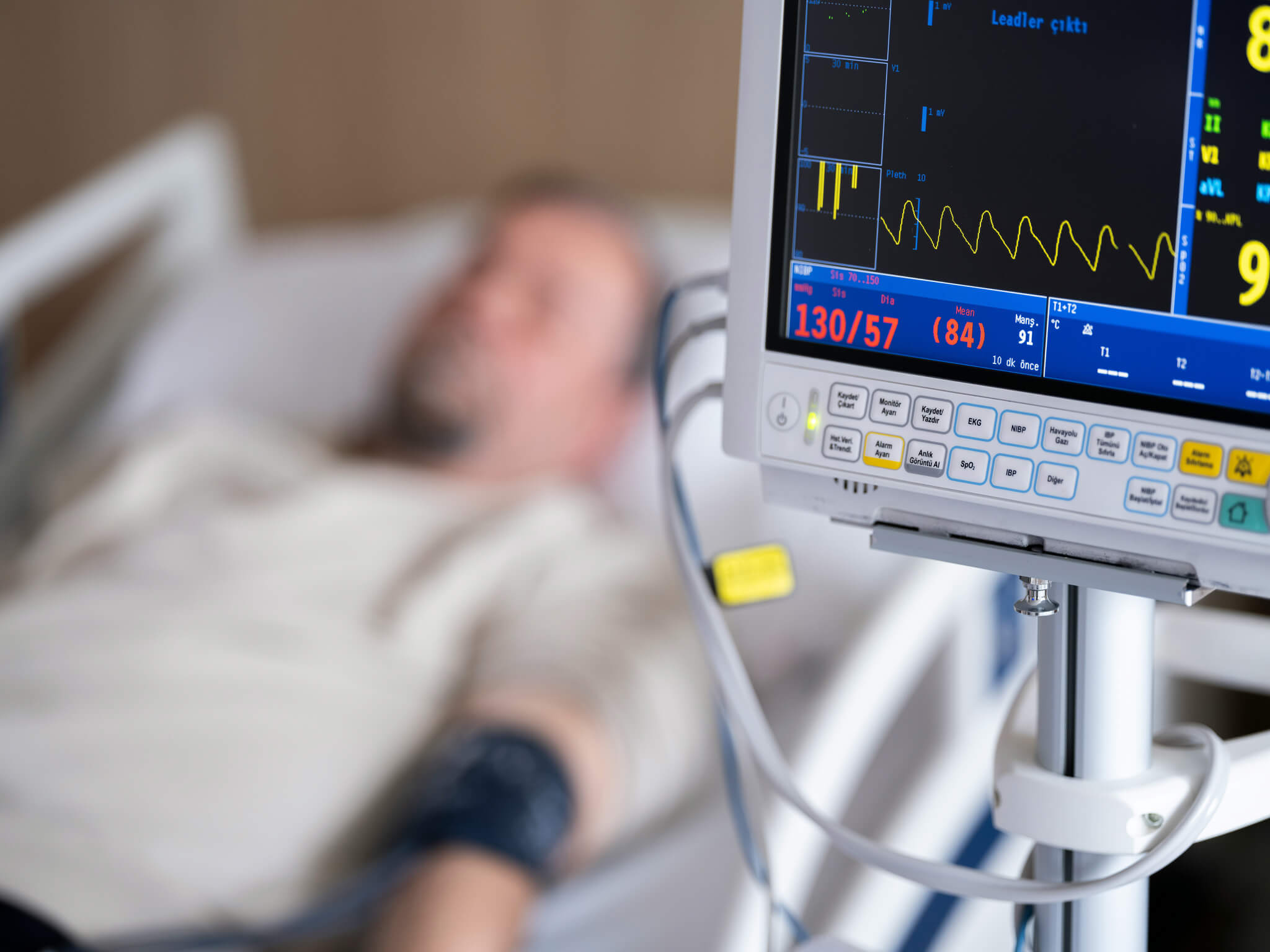
Stroke and neurological recovery
Although the brain is not the heart, stroke is closely linked to cardiology through common causes: atherosclerosis, atrial fibrillation, high blood pressure, and diabetes. Ischemic stroke occurs when a blood vessel in the brain becomes blocked and a portion of brain tissue is deprived of oxygen. Emergency treatment, thrombolysis or mechanical thrombectomy, is essential in the first hours.
In Romania, cerebrovascular diseases caused 42,826 deaths in 2023, representing approximately 14% of all deaths. Even more patients survive but are left with sequelae: speech difficulties, weakness on one side of the body, and problems with memory, attention, or orientation. Standard rehabilitation, such as physical therapy, speech therapy, and occupational therapy, is essential, but sometimes recovery reaches a plateau at a certain level.
Research on hyperbaric therapy for stroke has produced promising results. A study published in “PLOS ONE” included 40 patients with persistent neurological sequelae 6–27 months after stroke. The treatment protocol consisted of 40 hyperbaric therapy sessions of 90 minutes each, at 2 ATA. The results showed significant improvements in neurological function and quality of life in the treated group. SPECT imaging confirmed increased brain activity in areas with living but underfunctioning cells before treatment.
The medical explanation is related to what is called the “ischemic penumbra zone,” a region around the lesion that is not completely dead, but rather in a state of hibernation. These cells can survive in this state for a long time without functioning normally. Hyperbaric therapy delivers additional oxygen to them and may stimulate neuroplasticity processes, meaning the reorganization of the brain and the formation of new connections that take over affected functions.
Another study published in “Behavioural Neurology” confirmed that, after a protocol of 40 sessions, patients with ischemic stroke reported improvements in walking, strength, attention, memory, and sleep quality, improvements that were maintained 3 months after treatment completion. The message for patients and families is this: even if a stroke has passed the acute phase, the recovery window is much longer than previously believed, and hyperbaric therapy may contribute to additional progress.
Possible side effects: what is important to know
Like any medical procedure, hyperbaric therapy for the heart may be accompanied by side effects. The good news is that the most common ones are minor and temporary, while serious complications are extremely rare under appropriate medical supervision.
The most common side effect is discomfort in the ears or sinuses during the compression phases, similar to the sensation experienced on an airplane. It can be easily prevented and managed through simple equalization techniques. Patients with active respiratory infections are advised to postpone sessions until recovery precisely to avoid this discomfort.
Some patients experience mild fatigue or drowsiness after the session, which disappears within a few hours. There is also the possibility of temporary vision changes (transient myopia) in patients undergoing long series of sessions. These are reversible and disappear within a few weeks after the treatment ends.
Serious complications—pulmonary or cerebral oxygen toxicity—are extremely rare and are prevented through proper protocols: pressures and exposure times within safe limits, air breaks, and careful patient selection. Oxygen-induced seizures, for example, occur in fewer than 1 in 10,000 treatments.
At Hyperbarium, the prior medical consultation allows the identification of absolute contraindications (for example, untreated pneumothorax, certain chemotherapy drugs) and relative contraindications (severe claustrophobia, acute infections, uncontrolled epilepsy). Patients with cardiovascular conditions are carefully evaluated to ensure that the heart is stabilized before the protocol is initiated.
How to maintain cardiovascular health
No matter how valuable hyperbaric therapy may be as an adjunct treatment, its maximum effectiveness is achieved when the patient has also committed to essential lifestyle changes. Quitting smoking is probably the most important decision a cardiovascular patient can make, because smoking accelerates atherosclerosis, reduces the response to any therapy, and undermines the angiogenesis stimulated by hyperbaric therapy.
A Mediterranean or DASH-style diet, rich in vegetables, fruits, fatty fish, olive oil, whole grains, and low in saturated fats, sugar, and salt, is recommended by European cardiology guidelines for the secondary prevention of cardiovascular diseases. Likewise, controlling blood pressure, blood sugar, and cholesterol are basic requirements for recovery to progress.
Adapted movement—walking, breathing exercises, supervised physical therapy programs—rebuilds functional capacity and helps the heart adapt to exertion. A structured cardiac rehabilitation program under medical supervision reduces the risk of a new heart attack or cardiovascular death by up to 25–30% in the first years after the event, according to the guidelines of the European Society of Cardiology.
Emotional support matters too. Anxiety and depression are common after a heart attack or stroke, and they have a real impact on physical recovery. A patient who feels supported, informed, and involved in their own treatment recovers better. That is why, at Hyperbarium, the initial consultation is not just a medical formality, but a discussion in which the doctor explains what comes next, answers questions, and adjusts the plan according to each patient’s specific situation.

Why an individualized approach matters
Heart diseases are not identical from one patient to another. A young patient with a first heart attack who is otherwise healthy has a completely different profile from an elderly patient with chronic heart failure, diabetes, peripheral arterial disease, and multiple medications. The hyperbaric therapy protocol is adapted to each individual situation: pressure, session duration, total number of sessions, and frequency of administration.
At Hyperbarium, before starting any hyperbaric therapy protocol, each patient undergoes a thorough medical evaluation. This consultation includes reviewing diagnoses, medical history, current medication, and recent investigations. Based on this evaluation, the doctor decides whether hyperbaric therapy is indicated, whether additional investigations or medication adjustments are needed, and establishes the most appropriate treatment protocol.
The clinic’s medical staff has specialized training in hyperbaric medicine and experience gained in hospitals in Romania, Germany, and the United Kingdom. This is not a minor detail. Hyperbaric therapy in patients with cardiovascular diseases may require adjustments during the course, prompt recognition of unexpected reactions, and continuous adaptation of the protocol.
What hyperbaric therapy can and cannot do for the heart
It is important to be honest about what hyperbaric therapy can and cannot do. It does not reopen a completely blocked coronary artery. It does not replace a stent, eliminate the need for medication, or repair a structurally damaged heart valve.
What it can do, and what accumulated scientific evidence supports, is help tissues affected by lack of oxygen recover better. It can reduce the size of post-infarction lesions. It can support cardiac function in stable heart failure. It can stimulate the formation of new blood vessels in peripheral arterial disease and help prevent amputations. It can contribute to neurological recovery after stroke. It can improve the healing of ischemic wounds and diabetic foot ulcers.
It is a therapy with a biologically well-founded mechanism of action, with clinical studies showing positive results, and with a good safety profile when administered correctly. By definition, it is a therapy that complements, rather than replaces, everything modern medicine makes available for cardiovascular diseases.
Hyperbaric oxygen therapy for a healthy heart – additional support on the road to recovery
Cardiovascular diseases are a long and often difficult battle. But modern medicine today has more tools than ever before, and hyperbaric therapy is one of those that deserves to be known and considered where indicated.
The cardiovascular mortality rate in Romania remains concerning—2.5 times higher than the European average. This means that every therapeutic option that can support recovery, maintain quality of life, and reduce the risk of a new cardiovascular event is all the more important.
If you have gone through a myocardial infarction, if you are living with heart failure, if you have peripheral arterial disease, or if you are recovering after a stroke, hyperbaric therapy for heart diseases is a conversation worth having with your doctor. At Hyperbarium, the medical team can assess whether you are a suitable candidate, answer all your questions, and build together with you a therapeutic plan adapted to your individual situation.




